Copyright © 1999-2000 Samuel L. Baker
Sound instructions: Click the sound buttons to play the voice recordings.
Click again to stop the play.
If you are viewing this over a telephone modem internet connection,
playing the voice recordings involves loading delays of several minutes.
Cost-effectiveness analysis
(Continues the discussion from the presentation on cost-benefit
analysis.)
In this presentation:
-
Examples of cost-effectiveness analysis
-
Law of diminishing returns
-
Necessity for economic choice in health care
Cost-benefit and cost-effectiveness analysis -- the difference
Cost-benefit analysis
-
Both costs and benefits are evaluated in dollars and compared.
Cost-effectiveness analysis
-
The costs of alternative means of achieving some benefit are compared.
-
The benefit itself is not evaluated in dollars.
Cost-effectiveness analysis takes the objective -- the benefit --
as a given
With CEA, you seek the minimum-cost way
to meet the objective.
In health care cost-effectiveness analysis
- In health care CEA analyses, the goal is often in terms of
- lives saved,
- years of life saved, or
- quality-adjusted years of life saved
-
A better way to think about this would be reduction of risk -- for example,
finding how to get the most risk reduction per dollar spent -- but I haven't
seen that done in any actual studies. (We'll come back to this point in the following discussion.)
Neuhauser and Lewicki's Stool Guaiac article
Neuhauser, D., Lewicki, A.M., "What Do We Gain from the Sixth Stool Guaiac?"
N Engl J Med, July 31, 1975, 293(5), pp. 226-228.
I recommend you follow along with the article itself.
Guaiac
Guaiac is short for guaiacum, tree that grows in the West Indies and tropical
America. Its resin turns black if mixed with blood.
It's used to detect colon cancer by looking for blood in the stools.
Sensitivity and Specificity
The table below shows the four possible combinations of actual disease
state (the patient either does or does not have the illness) and test result (positive +
or negative -).
In the tables below, to save space, a + sign means a positive test result, meaning
that the test found evidence of the illness. A - sign means a negative test result,
meaning that the test found no evidence of the illness.
In the table, green represents a correct ("True") finding. Red
represents an incorrect ("False") finding.
|
Test result
+ |
Test result
- |
| Patient has the illness |
True + |
False - |
| Patient doesn't have the illness |
False + |
True - |
Sensitivity = (True +) / (People with illness)
Sensitivity is how many of the sick get found.
Specificity = (True -) / (Patients without illness)
Specificity is how many of the well are correctly so identified.
This specificity formula was corrected after the 2000 sound files were recorded.
Senstivity of the Guaiac Test
The test is positive in 11 out of 12 people who have colon cancer developing.
Sensitivity of repeat tests
Let's accept the authors' assumption that the repeat tests are independent.
- Independence means that if someone has cancer and is unlucky enough
to have a false negative on one test, the probability of a true positive
on the next test is still 11/12.
Based on that assumption, we can construct this table:
The third column represents 1/12 raised to
a power equal to the number of tests for that row. This is the
probability of a person with cancer being missed on every test taken.
Subtract those
numbers from 1 to get the decimals in the second column. They are the probabilities of not being missed.
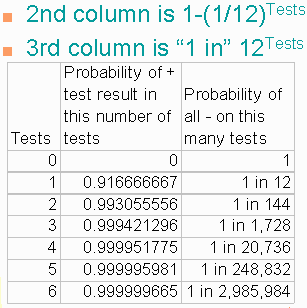
Perfect sensitivity can't be achieved
You can reduce the number of misses by repeating the test.
With 2 tests you miss only one cancer in 144,
With 6 tests you miss only one cancer in 2,985,984.
However, no matter how many times you repeat the test, you can't reduce
the misses all the way to 0.
The marginal contribution of each test
For illustration purposes, the authors base their calculation on a population
of 10,000.
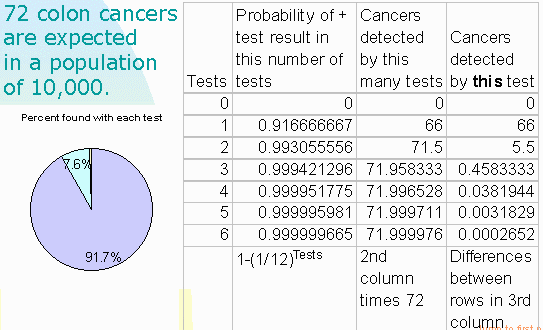
Law of diminishing returns
In this example:
Each test adds to the number detected,
but each successive test adds fewer detections than the test before
it did.
Economists say: The return from successive tests diminishes.
Law of Diminishing Returns
In general, for consumption goods (or services):
The more you have of something, the less benefit you gain from having
one more of it.
It can be called the Law of Diminishing Marginal Returns, because it's
saying that:
The marginal benefit of a good diminishes as you get more.
-
Marginal benefit = added benefit from one more.
The moral problem:
Every successive test has some marginal value, but the marginal value diminishes
with each test.
Where do you stop? You can't simply say: Do all you can for the patient.
No matter how many tests you do, the next one might still pick up a
cancer that the others missed.
Similar issue in pollution control, food additive regulation, etc.
How many tests would you recommend?
Here's the table again.
Please write down how many tests you would want.
-
I'll ask you again after we go through the analysis.
-
By the way, before this article was published, the American Cancer Society
was recommending 6 tests. That is why this article's tables have rows
for 6 tests.
Costs for repeated guaiac tests
For a population of 10,000, the costs are shown in the table below.
In the table, the cost per test goes down for successive repetitions
because, as mentioned, people testing + on one test aren't tested again.
The costs shown in the table include the costs of follow-up tests (barium
enema) for people with positive guaiac results. Many of those positives
are false. The false-positive rate is 3%.
Column 1:
Tests |
Column 2:
Total Cost |
Column 3:
Average Cost |
Column 4:
Marginal Cost |
| 0 |
$0 |
--- |
--- |
| 1 |
$77,550 |
$77,550 |
$77,550 |
| 2 |
$107,756 |
$53,878 |
$30,206 |
| 3 |
$130,283 |
$43,428 |
$22,527 |
| 4 |
$148,217 |
$37,054 |
$17,934 |
| 5 |
$163,255 |
$32,651 |
$15,038 |
| 6 |
$175,749 |
$29,292 |
$12,494 |
|
|
2nd column divided
by first column |
Difference between each row's total cost
and the row above it's total cost |
CEA the wrong way, using the average cost
| Tests |
Cancers detected by
this many tests |
Total cost
of this many tests |
Cost per detection |
| 0 |
0 |
$0 |
--- |
| 1 |
66 |
$77,550 |
$1,175 |
| 2 |
71.5 |
$107,756 |
$1,507 |
| 3 |
71.9583 |
$130,283 |
$1,811 |
| 4 |
71.9965 |
$148,217 |
$2,059 |
| 5 |
71.9997 |
$163,255 |
$2,267 |
| 6 |
72 |
$175,749 |
$2,441 |
|
|
|
3rd column entry divided by
the 2nd column entry |
This table suggests that the average cost per detection goes up with the
number of tests, but not by very much. Doing 6 tests finds cancers at a
modest cost of $2,441 per detection.
This makes doing 6 tests look like a good investment. Actually, though,
the method is faulty. Average cost does not help you decide whether the
sixth test is specifically worth doing.
CEA the right way, using the "marginal" concept
Notice that in the table below it says "this test."
Compare the table above, where it said "this many tests."
That's the difference between marginal and average.
| Tests |
Cancers detected
by this test |
Marginal cost
of this test |
Marginal cost per detection |
| 0 |
0 |
--- |
--- |
| 1 |
66 |
$77,550 |
$1,175 |
| 2 |
5.5 |
$30,206 |
$5,492 |
| 3 |
0.458 |
$22,527 |
$49,150 |
| 4 |
0.038 |
$17,934 |
$469,545 |
| 5 |
0.003 |
$15,038 |
$4,724,666 |
| 6 |
0.0003 |
$12,494 |
$47,104,652 |
|
|
|
3rd column divided by
2nd column |
Now we see that the marginal cost per detection goes up rapidly with the
number of tests.
The 6th test costs $47 million per case detected. Wow!
In view of these numbers, how many tests would you recommend?
Is your answer any different now? Please report both of your answers
in your comment, even if the main subject of your comment is something
else.
CEA and CBA
At this point, we could do a cost-benefit analysis (CBA) by setting a dollar
value on a detected cancer. We would then chose the highest number of tests
with marginal cost per detection less than the value of a detection.
Instead, for a cost-effectiveness analysis, we can compare these costs
per detection with the costs of other life-saving measures.
Still thinking about how many tests to recommend?
When making your recommendation, please assume, as Neuhauser-Lewicki do,
that a cancer detected is a life saved.
Then consider that renal dialysis (keeping someone alive by kidney machine)
costs upwards of $50,000 per year. If your maximum acceptable cost per
detection is less than $50,000, then you are implying that kidney machines
are a waste of money.
Also consider that a couple of years ago, a town in the U.S. spent over
$1 million to dig a trench to rescue a child who had fallen into a well.
If your maximum acceptable cost per detection is less than $1 million,
then are you implying that the people in that town wasted their money?
(After the devastating 1999 earthquake in Turkey, and the 2010 earthquake in Haiti, those countries were unable to spend anything close to that much per person to rescue people
from collapsed buildings.)
Saving statistical lives vs. saving identifiable lives
It does seem generally true that we spend more for saving identifiable
individuals.
See T.C. Schelling, "The Life You Save May Be Your Own," in S. B. Chase,
ed., Problems in Public Expenditure Analysis. An abridged version is in
Dorfman and Dorfman, eds., Economics of the Environment, 3rd. ed.
Risk -- a better approach
Neuhauser-Lewicki's cost per cancer detected criterion is not strictly
correct, because it ignores risk aversion.
What is the test's real benefit?
-
The lives saved?
-
No. This would mean the test only benefits the few who have a
cancer detected.
-
This test benefits everyone who takes it by reducing his or her risk of
having an undetected cancer.
-
The test's real benefit is therefore the risk averted.
Risk aversion
It is not irrational to fear risk.
-
Though it is irrational to exaggerate risk.
The fear of risk is why people buy insurance.
People pay to avoid risk, which implyies that the total disutility
of the risks of all the bad events is greater than the total disutilities
of the bad events themselves.
-
The risk aversion concept is explained at length in an interactive lecture that is coming soon on the
syllabus.
Analysis using risk
The correct method would be to ask if it is worth an expected $1.25 ($12,495
/ 10,000),
-
plus time and inconvenience
to reduce your probability of having an undetected cancer by about 1 chance
in 38,000,000.
-
1 in 38 million is the probability that
-
a person in the prime age group has cancer AND
-
is negative on 5 tests AND
-
shows positive on the sixth test.
Guaiac test cost-risk table
| Tests |
Among those with colon cancer, the probability benefiting from this
test (all - on tests before, then + on this test) |
The probability that you will benefit from this test. (2nd column times
72/10000, the rate of colon cancer in the population.) |
The expected marginal cost of this test. |
| 0 |
0 |
0 |
|
| 1 |
1 in 1.09 |
1 in 152 |
$7.76
|
| 2 |
1 in 13 |
1 in 1,818 |
$3.02
|
| 3 |
1 in 157 |
1 in 21,818 |
$2.25
|
| 4 |
1 in 1,885 |
1 in 261,818 |
$1.79
|
| 5 |
1 in 22,621 |
1 in 3,141,818 |
$1.50
|
| 6 |
1 in 271,453 |
1 in 37,701,818 |
$1.25
|
What the guaiac test example shows
-
An economic decision is unavoidable.
-
Even a cheap test can be very expensive, in terms of its cost-effectiveness.
-
How easy it was for the health care system to overspend.
After this article came out, the American Cancer Society reduced its recommended
number of tests.
E-mail:
The views and opinions expressed in this page are strictly those of the
page author. The contents of this page have not been reviewed or approved
by the University of South Carolina.


